Rehab Management spoke to a longtime physical therapist at an acute care facility to find out what’s new in the landscape of inpatient stroke rehabilitation.
By Steven Martinez | Photos by Karen Ingham and Dave Kinney
Each year nearly 795,000 people have a stroke in the United States, and while rates have plateaued in recent years there is a worrying uptick in the number of strokes for Americans under the age of 50, according to the American Stroke Association.
The Centers for Disease Control’s (CDC) most recent estimates show that strokes carried an economic cost of nearly $53 billion in both direct costs and lost productivity, placing a heavy burden on patients and their families as well as their communities.
But aside from the financial costs, a stroke can also rob people of their physical and mental identities. The suddenness of the sea change, coupled with the daunting task of regaining a semblance of their former lives, presents a challenge for both patients and their caregivers.
New innovations in robotics, virtual reality, and other technologies have given therapists more tools to help stroke sufferers regain some of their mental and physical abilities. But stroke patients and therapists still face an uphill battle in their wellness journey.
On the front lines of this battle is Stephanie Zanvettor, PT, CBIS, CCI, a physical therapist at Gaylord Specialty Healthcare in Wallingford, Conn. We talked to Zanvettor to get her take on the trends in inpatient stroke rehabilitation and new technologies they are using to facilitate recovery.
Rehab Management: What are some of the really new technologies and treatments that your facility is using for inpatient stroke rehabilitation?
Stephanie Zanvettor, PT, CBIS, CCI: In general, some of our newest acquisitions for technology include the following:
- a body weight supported harness system.
- an upper body robotic device to assist the upper extremity in recovery
- a multi-disciplinary tool used to facilitate recovery with emphasis on vision, use/control of the upper extremity and the balance system to work on balance.
- a tool used by our speech pathologists to visualize swallow activity
- a lower extremity device used to assist with addressing foot drop post stroke recovery.
- a virtual reality system that helps stroke survivors with balance and coordination through a variety of experiences.
RM: Can you tell me a bit more about some of these technologies?
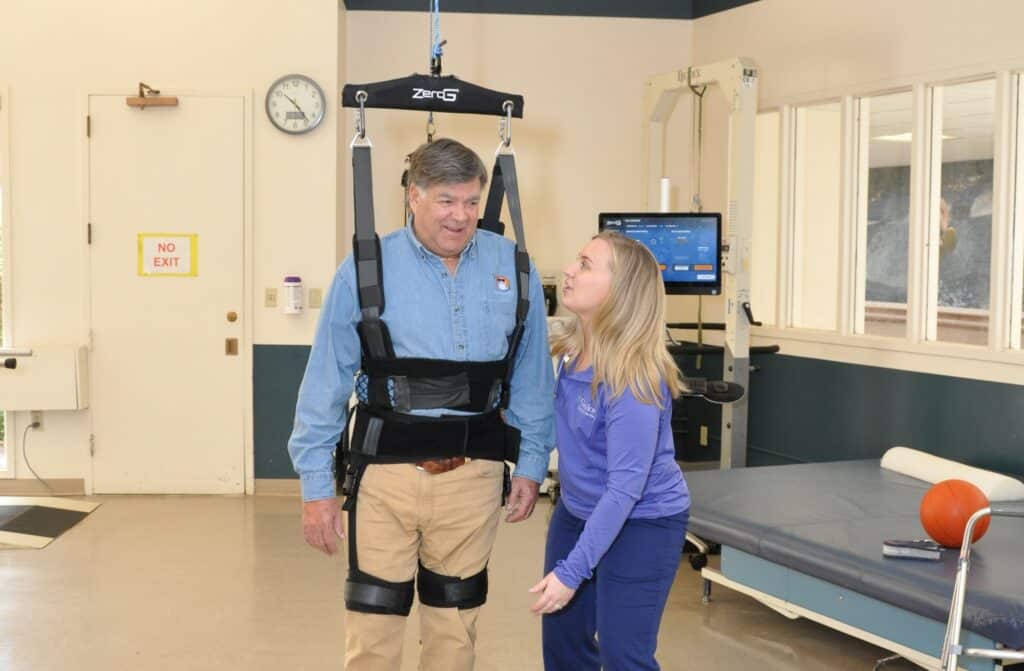
Zanvettor: Our body weight supported harness system is utilized many times with physical therapy and/or occupational therapy to co-treat and work with individuals that require a significant amount of physical assistance for standing or gait training. Using some of the specific programs within the system, we also will place individuals that are ambulatory, or already walking, into it to work with them on progressing their bounds and helping them to a full recovery. There are different functions you can use including all kinds of balance exercises.
Our upper extremity robotic device is actually pretty new. It’s utilized predominantly by our occupational therapists, who use it to work with patients that have hemiparesis or weakness in their arms to regain both range of motion and strength.
It’s very engaging. Like a lot of robotic technology these days, particularly upper extremity robotics, this system uses a gaming pattern, [with interactive games on a screen guiding their movements]. So, for example, somebody who has no movement in their arm might use the device to work on range of motion at the shoulder and the elbow. Someone else who has some movement in their arm, even if weak, might use it to work on things like hand-eye coordination, being able to bring their supported arm to a particular target on the screen in front of them.
RM: In the 12 years you’ve worked at Gaylord, how have these new technologies affected your approach in therapy?
Zanvettor: When I first started working as a PT, we didn’t have half of the things that we have now. Did we get by? Sure. With respect to the concept of upper extremity robotics, they had that in its infancy stages when I was a newer PT but there’s more on the market now, so it’s becoming a hotter thing. Same thing with respect to the overhead type of gait training devices.
But overall, yes, I would say that we are very fortunate at Gaylord to have access to a number of these devices. Certainly, they are used pretty regularly with our patient population and in working hard to get our patients better.
There’s a lot more technology out there, but some of these devices can be quite expensive and that is the reason why many facilities don’t have them.
RM: How have things changed in recent years for stroke patients when it comes to rehab?
Zanvettor: In general, the acuity of our stroke patients has changed over the years and we are seeing changes in the insurance companies’ support for stroke rehabilitation. We get many denials of coverage and shorter lengths of stay. This combination has forced clinicians to think and treat creatively as our length of stay for this population has suffered. We are in the position to offer as much as we can in the time that we have our patients.
We are also seeing an increase in our young stroke survivors (not just by age, but those working or who are caregivers at the time of their stroke), as well as an increase in the number of patients requiring telemetry monitoring post stroke.
RM: Why do you think that insurance companies are backing away from their support of inpatient stroke rehabilitation?
Zanvettor: Our stroke survivors are staying with us for three to four weeks. What we’re seeing now is that we get a number of insurance denials for various reasons, depending on the insurance company.
To be honest with you, I don’t know what it comes down to. Our care managers are the ones having to deliver the news to the individual, who are often disheartened to hear that their stay has been challenged by an insurance company. That never makes people feel good. Care managers are the ones going to bat for patients and staff in trying to help us justify keeping the patients here.
I’ve had patients that have been here for a couple of weeks and then insurance companies are knocking on the door saying, “OK, time for them to transition onward.”
Many times, it’s linked to the idea that Gaylord is a long-term acute care hospital. Not every stroke patient in the state of Connecticut comes to Gaylord, and that’s because medically they need to qualify to come here. From an insurance company’s perspective, once an individual is deemed medically stable then, regardless of their rehabilitation needs, they want that person to transition to a subacute or skilled nursing facility.
Lately, as of the past several years, we are seeing stroke patients coming in at much lower levels functionally than they were previously. Our patients are sicker. They have many more additional medical comorbidities. A lot of them come in on telemetry.
Our patients are coming to us weaker and with a shorter length of stay. It has complicated things for us to get them further along in their rehabilitation before they have to make that transition.
RM: You mentioned that insurance issues and shorter stays were forcing clinicians to be creative with their treatment. Can you provide an example?
Zanvettor: There’s a lot of research right now supporting the use of high-intensity gait training with stroke survivors. That’s getting folks up and moving and challenging them in such a way that their heart rate is able to reach a targeted range that’s an age-based number. We are using technology to help achieve that goal more quickly.
As an example, let’s take a patient who can walk outside of the weight supported harness system with a walker or cane but can only make it 50 feet before they fatigue. If I, from a creative perspective, place that individual in the harness system where they have a little bit of weight supported — which might help them if they have arthritis or pain in their knees — I might be able to get them walking longer distances before they need to take a rest.
RM: So you can get the most out of your time with them?
Zanvettor: Yeah, certainly. Given the adjustment to lengths of stay and individuals coming in at a lower functional level, we are utilizing these devices to the best of our ability.
We use devices like the upper extremity robotic device to regain arm function, as opposed to just doing simple range of motion with exercises in bed. The devices also help keep patients engaged and wanting to participate. You get a little bit more out of them if they’re engaged.
We have other types of technology here like virtual reality. For example, maybe somebody was an avid golfer prior to their stroke and that’s something that they very much enjoyed doing. Our therapeutic recreation department might pair up with our occupational therapist or physical therapist and get them into virtual reality to practice a golf swing or something of that nature.
RM: Can you expand on how you use virtual reality?
Zanvettor: Our virtual reality system is beneficial to patients and allows them to choose their experience and work on functional skills in a seated or standing position.
I think a lot of it goes back to making a connection with the patient, from a recreational perspective, to the activities they once enjoyed and tying it into a therapy session. Whether it’s guided meditation, using it as a game, or if it’s from a functional perspective, working on balance, developing strength, or working on coordination, it’s about being able to work in a therapeutic way without it feeling like a therapy session.
You exercise when you’re on a golf course if you’re walking the course and swinging your club, but are you necessarily thinking about it as if you were on a treadmill? So, it’s about finding an activity that an individual enjoys and using that activity in a therapeutic way to help them exercise without thinking about what they’re doing.
I haven’t personally used virtual reality all that much. That’s predominantly used here with our therapeutic recreation folks, but certainly from a PT perspective and OT perspective, they can pair up with them to utilize the device.
RM: We’ve seen some futuristic technologies make their way into the rehabilitation market, including exoskeletons. How is this type of technology helping you to treat patients?
Our exoskeleton has many uses in stroke recovery. It is beneficial to those that require a significant amount of assistance for gait/standing, working on transfers (specifically sit to stand), weight shifting and weight acceptance (both necessary components of gait training post-stroke), as well as strengthening of hemiplegic lower extremities. The exoskeleton is also beneficial to individuals post-stroke who suffer from difficulties with spatial and midline orientation.
An exoskeleton is great for folks who are not necessarily ambulatory and it’s also beneficial to those who might be ambulatory if we’re working on increasing endurance for stepping or working on strengthening of a hemiparetic leg or something of that nature.
Sometimes after a stroke, someone who presents with difficulty in spatial orientation and midline will use their strong side to push toward their weaker side. The term for this is lateropulsion or pushing. How we use the exoskeleton with those individuals is that we’ll get them up and in the suit and have them standing and use a tool within the system to work on some biofeedback.
The tool offers a view of where they are standing and uses tones and auditory response as feedback. Then we work with the patients on shifting their weight and they can see a dot move on the screen in front of them coinciding with their movement. They can use the dot to see which side they’re moving to and listen to the tone to tell them where they need to stay.
Using the exoskeleton and the programming within it to work with these individuals on their spatial awareness, spatial orientation, and weight shifting activities can help facilitate gait transfers and any other mobilization.
RM: When you are rehabbing stroke patients, regardless of the technology you are using, what is the main goal for your team and how would you define successful inpatient stroke rehabilitation?
Zanvettor: Our main goals in an inpatient rehab setting are to assist our patients with achieving the functional goals required for a successful transition to home (for those who are able to return home) and for those who are not able to return directly home, reducing the burden of care to achieve the highest level of function possible.
RM: How much of rehabilitation is dependent on the patient’s own attitudes?
Zanvettor: Attitudes toward recovery and the survivor’s own thoughts on dealing with health issues certainly play a role in recovery. As does the nature of stroke. No one elects to have a stroke. They occur without warning and are unwanted. Therefore, some survivors do face challenges in their recovery that impact their participation in therapy.
We use a scale to assess this impact called the Apathy and Engagement Scale. We work with patients to identify what their goals and interests are and thus guide our therapy sessions around what the individual stroke survivors’ goals are to foster rapport and increase participation.
RM: How might you find success with a patient who is not making the process easier?
Zanvettor: We have many tools at our disposal to foster building a rapport with our patients and thus working with the survivor in their recovery. We use “Get to Know Me” sheets to assist with identifying an individual’s likes and dislikes. Then we use our technology to facilitate our patients with achieving their specific goals.
Steven Martinez is the associate editor for Rehab Management. For more information, contact [email protected].




