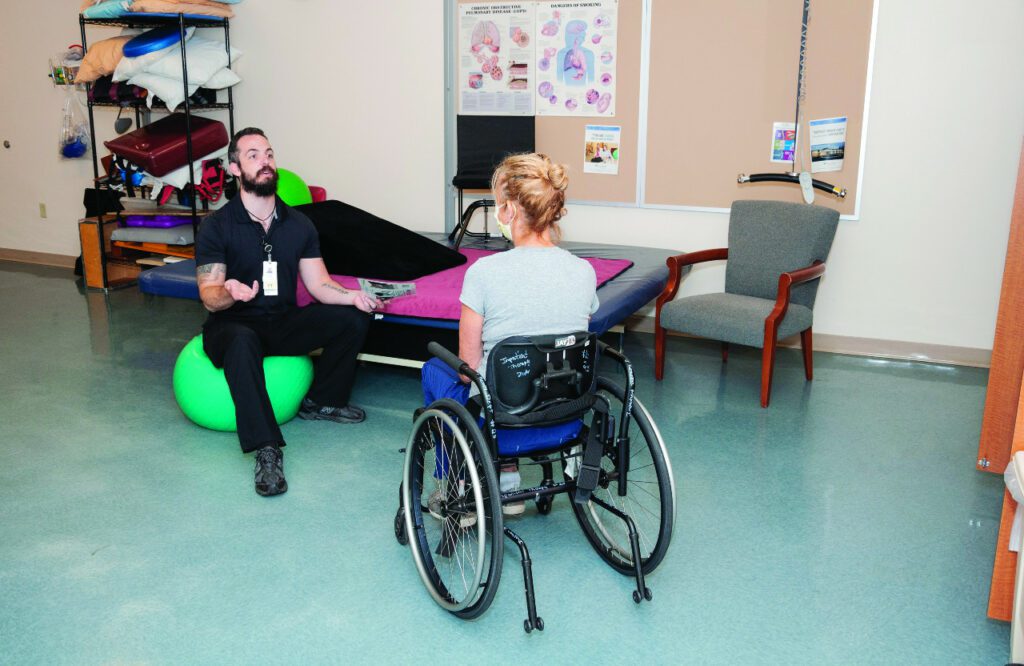
PHOTO CAPTION: Comprised of physiatrists, physician assistants, occupational therapists, physical therapists, social workers, nurses, and care managers, Gaylord’s SCI Sexuality Committee reviews intake questionnaires to create custom consultations based on a patient’s own interests and goals. Photo: Karen Ingham Photography.
Spinal cord injuries have a profound effect on all aspects of a person’s life.
By Timothy Kilbride, PT, DPT
When a therapist meets a person with a new injury or dysfunction, they embark on a journey to teach that individual an entirely new set of life skills that will challenge them physically, mentally, and emotionally. There are many unique challenges that come with spinal cord injuries that need to be addressed precisely and in great detail, but one topic that is all-too-often left out of the conversation is sex.
Throughout my career as a physical therapist, I have witnessed many patients’ questions about sex and spinal cord injuries being met with half-answers, quick topic changes, or the infamous reply, “You’ll work that stuff out when you get back home.” As a healthcare provider, these responses are both disappointing and jarring to hear. Can you imagine sending a patient home with a catheter, no training, and assuring them that they will be able to work it out when they get back home?
As therapists, we need to ask ourselves, “Why has sex become the forgotten ADL?” More importantly, we need to ask ourselves the same question that all healthcare workers ask themselves each day: “How can we do better?”
A Fundamental Part of Being Human
Our sexuality is fundamental to being human. I am talking about not only the act of having sex, but our self-image as sexual beings, our emotional connection to other people, and, of course, procreation.1
Who we are as sexual beings stems from our brains. A spinal cord injury doesn’t change that. There are many commonly held assumptions that people with spinal cord injuries are inherently uninterested in sex, can’t have children, don’t have the capability to have sex, and are no longer desirable partners.2 All of these things could not be further from the truth.
In my experience, the under-addressed issue of sexuality stems from a combination of social taboos, a dearth of information, feelings of discomfort, and poorly defined roles of who exactly should broach the subject first. Often the topic is avoided or only spoken about if it “happens to come up.”
Evidence shows that if a rehabilitation team does not first address the topics of sexual desires, needs, and functioning with spinal cord patients, then the patient will avoid asking questions.2 It makes sense…why should a patient feel comfortable asking about sex if their healthcare team does not?
An Interdisciplinary Solution
As an inpatient physical therapist at Gaylord Specialty Healthcare, a long-term acute care hospital headquartered in Wallingford, Conn, I work every day with people who have experienced life-altering spinal cord injuries. I noticed that aside from a generic 20-minute discussion during our spinal cord injury education series, little information was available to those patients interested in finding adaptive ways to continue to be sexually active after their injury. Patients were going home with more questions than answers about a very important part of their identity and their body’s functionality.
Convinced that this was an important topic that needed to be addressed with each patient, I assembled a team of specialists whose enthusiasm, unique knowledge, and expertise would prove invaluable to filling this unmet need. Physiatrists, physician assistants, occupational therapists, physical therapists, social workers, nurses, and care managers soon crowded around tables at lunchtime to brainstorm ways to solve this decades-long dilemma. Each member of the interdisciplinary committee brought a unique perspective: from clinical staff who regularly treat newly injured people, to a staff member who serves on the board of the local chapter of the United Spinal Association who offered insight from members of the SCI community.
What started as a simple idea took off. Thanks to a grant obtained by Gaylord Specialty Healthcare’s development staff, we were able to procure a range of adaptive equipment, devices, and various manuals that would prove to be valuable educational tools. Our committee members spent hours scouring various resources and texts to ready ourselves to discuss a number of topics ranging from erectile dysfunction and fertility to sex positions, adaptive equipment, and much more.
PLISSIT Model of Education
Gaylord’s goal was to develop a program that offers people with spinal cord injuries or dysfunctions and their partners the opportunity to find information that is highly tailored to their specific interests, questions, and needs. After months of thoughtful debate and information gathering, our committee decided to base our education on the PLISSIT model (permission, limited information, specific suggestions, and intensive therapy3). This structure works well to provide the information that a patient is interested in learning without the concern of overwhelming them or venturing into territory that may be uncomfortable or traumatic.
The topic of sexuality is initially broached as a subject during Gaylord’s SCI education series. This step allows the patient to consider the topic along with the offer of additional consultations with the team. If a patient decides that they would like to take advantage of our program, they are given an intake questionnaire to select which topics they are interested in, which topics they would like to avoid, what gender and sexual orientation they’d prefer their team members to be, and any other people such as partners or caretakers they would like to attend the session with them.
Armed with this information, we are able to schedule the patient for a consultation with the most appropriate team members. If, for example, a patient has questions about how to get into certain positions, which adaptive equipment is best for their injury, or how to put on a condom with limited hand function, the team might consist of a physical therapist and an occupational therapist. If the patient has questions about mixing a drug for erectile dysfunction with their current medication or the risks of blood clots with birth control combined with an SCI, the team might consist of a nurse and a physician.
A Case Study in Quality of Life
One of the first clients to avail himself of Gaylord’s education program was a gentleman whom we will refer to as “AL,” and his case study is a fantastic example of how our interdisciplinary team worked to create a custom program suited to our patients’ needs and interests.
AL sustained a C6-C7 ASIA B injury about 1 year before his initial consult with Gaylord’s team. AL had already returned to sexual activity since his injury but strongly felt that having additional education would be immensely helpful.
After reviewing his intake questionnaire, the committee assembled a team consisting of a physiatrist to address medication questions, a physical therapist to help problem-solve transitioning in and out of various positions with his new diagnosis of heterotopic ossification (bone growth in his muscles and tendons), and an occupational therapist to offer suggestions about adaptive devices and equipment. Once AL noticed our staff’s ease in speaking openly, he also began to feel at ease. The conversation flowed organically with one question leading into another, leading into even more in-depth questions.
We began talking about his current sex life and goals that he had for improvement, then moved on to alternative options for erectile issues (he was currently using injections, so we discussed other options to bring to his urologist), then to positioning equipment that would allow him to be more participatory during sex even with his newly restricted range of motion. Between pulling up instructional videos, demoing equipment, answering questions, and, of course, laughing, an hour passed in the blink of an eye.
AL was able to take our ideas, try what he could at home, and then come back and let us know what went right and what went wrong. Together with feedback from our patient and his partner, we were able to troubleshoot and find other solutions where possible.
Improved Quality of Life for Patients and Their Partners
The positive feedback received from all of the patients who have taken advantage of Gaylord Specialty Healthcare’s unique program affirms the great need for this type of education. Plans are currently underway to make the program available to the community on an outpatient basis.
Sexuality is a normal part of being human, and a spinal cord injury or dysfunction should not be a barrier to its enjoyment. As healthcare workers, it is our duty to make sure that we do better in the future for our patents’ sake.
Sex is a topic that healthcare providers must become more comfortable talking about, and efforts should be taken to more fully integrate the topic into spinal cord injury rehabilitation programs and educational materials. We simply can’t afford to let it remain the forgotten ADL. RM
Timothy Kilbride, PT, DPT, is a Level III inpatient physical therapist for Gaylord Specialty Healthcare, Wallingford, Conn. Kilbride received his Bachelor of Health Science and his Doctoral Degree in Physical Therapy from University of Hartford and has been working with patients with spinal cord injuries and dysfunction for over 10 years. For more information, contact [email protected].
References
- Kaufman M, Silverberg C, Odette F. The Ultimate Guide to Sex and Disability. San Francisco, 2003:1-26
- Somers M. Spinal Cord Injury: Functional Rehabilitation Third Edition. Upper Saddle River, New Jersey, Person Education Inc, 2010:348 – 365
- Annon J. The PLISSIT model: A proposed conceptual scheme for the behavioral treatment of sexual problems. J Sex Ed Ther. 1976;2(1):1-15




