Occupational therapy helps restore function to patients with upper limb loss
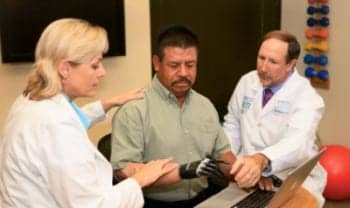
Prosthetists and occupational therapists work closely with upper limb patients to help restore functional ability. (All photos courtesy of Advanced Arm Dynamics.)
Patients with upper limb amputation or congenital limb difference represent a unique population with specific rehabilitation needs. As with any diagnosis, it is important to provide therapeutic intervention within an overarching framework of rehabilitation specific to this patient population. Utilizing this framework, the therapist can begin to develop a treatment plan based on protocols specific to the level of limb loss and further refine the plan to meet the patient’s individual needs.
In the United States, there are approximately 1.7 million people living with limb loss.1 It is estimated that one out of every 200 people in the United States has had an amputation.2 Dillingham et al examined hospital discharge data from 1988 to 1996 to develop estimates of the annual incidence rate of limb loss and congenital limb difference in the United States. The data revealed an average rate of 133,235 limb loss discharges per year. Amputations of the upper limb (disregarding amputation of the fingers, thumbs, toes, and foot) occurred at a ratio of 1 upper limb amputation to approximately 35 lower limb amputations.3 Of the upper limb amputations occurring annually, 91% are distal to the wrist and 9% are proximal to the wrist.
The primary cause of upper limb amputation was trauma (78.9%), while the primary cause for lower limb amputation was vascular disease secondary to diabetes (92.7%). Secondary causes for upper limb loss were vascular disease (17.2%), congenital limb difference, and cancer. Secondary causes for lower limb loss were trauma (6%), cancer, and congenital limb difference.3
UNIQUE NEEDS REQUIRE A SPECIALIZED TEAM
While the incidence rate of upper limb loss is small in comparison to lower limb loss, this patient population requires a complex level of care and rehabilitation. Therapists who specialize in upper limb loss and rehabilitation are acutely aware of the inherent psychosocial, physical, and functional issues that may be present. The effects of living with upper limb loss often amplify these issues and require specialized intervention.
It is essential to develop a comprehensive approach to rehabilitation that involves a team of health care professionals working in partnership with the patient. The medical team will certainly include the physician, nurse, social worker, therapist, and prosthetist. Ideally, the team also includes professionals to address case management, psychosocial, and nutrition concerns.
All team members must have a basic understanding of the course of intervention for prosthesis fitting and therapeutic training for functional use. Therapists may encounter upper limb prosthesis candidates at any point in their recovery process. If possible, it is most advantageous for the therapist to be an active participant from the outset of medical intervention. A therapist’s training and professional perspective prove to be invaluable to limb loss patients for many reasons throughout the rehabilitation process. Therapists may address the following: wound care, scar management, orthopedic disturbances, overuse of the sound limb, ergonomic adaptations, functional activity training, patient and family education, and training to prepare the patient for use of a prosthetic device. Therapists also serve as patient advocates throughout the continuum of care.
PROSTHETIC REHABILITATION LEADS TO AN ACTIVE LIFE
Upper limb loss secondary to traumatic injury is often the result of on-the-job accidents. Shawn Findley was working on a punch press in an industrial fabrication shop when a portion of his hand was amputated by a machine. In an attempt to save what remained of his injured hand, Findley endured 13 surgical procedures, only to still be faced with persistent pain and a partial hand that offered minimal function. He consulted with an upper limb prosthetist and occupational therapist to learn about the prosthetic options that would be available if he decided to have the injured hand amputated.
Three years after his injury, Findley decided to have his hand amputated. This was the pivotal point in his return to a productive and fulfilling lifestyle. Once this decision was made, his surgeon, prosthetist and OT collaborated with him to discuss his functional goals and how he saw himself using a prosthesis. He determined that he would benefit from a myoelectric prosthesis with a custom cosmetic covering for many of his activities of daily living. He also chose an activity specific device to enable him to participate in coaching soccer, baseball and basketball for his children again.
It is ideal to engage in this collaborative process prior to amputation and provide information to the surgeon to determine the optimal level of amputation for successful prosthesis use. Preserving length is not always the surgeon’s guide. Other important considerations include allowing room for use of prosthetic components and the patient’s ability to activate forearm muscles for myoelectric control.
Findley’s OT tested and identified adequate myoelectric muscle sites (wrist extensors and flexors) and began training the muscles for use. After an extended period of inactivity, Findley’s muscles had atrophied considerably. Training muscle facilitation before and after amputation strengthened these muscles for independent control of opening and closing a terminal device once he was fit with his first prosthesis.
After amputation and preparatory prosthesis training, Findley was pain-free and began to gain more independence in self-care and higher level bi-manual tasks.
GENERAL REHABILITATION FRAMEWORK
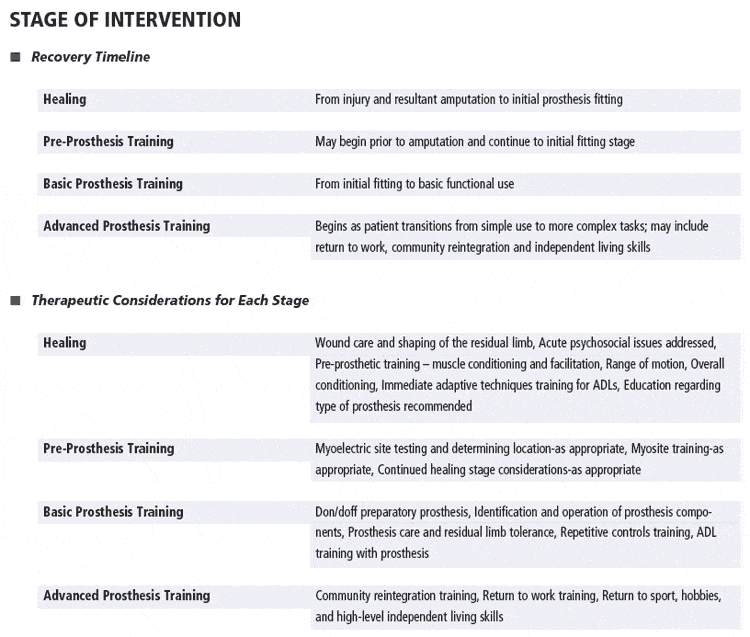
The upper limb prosthetic rehabilitation process is organized into broad segments that help give focus and continuity to the long-term treatment plan. These segments are not finite and may overlap. Smurr et al characterize these stages as follows:
PROSTHETIC REHABILITATION HELPS RESTORE INDEPENDENCE
In cases of bilateral upper limb loss, prosthetic rehabilitation is critical to restoring some degree of independence to the patient. During the initial stage of rehabilitation, without one sound hand to assist them in their daily life, the patient is completely dependent on someone else for their most basic and personal needs such as toileting, bathing, dressing, and eating.
Electrical lineman Cliff Anderson experienced bilateral arm amputation at the shoulder in January 2012 after he was electrocuted while working at a transformer station. Comorbidities include severe burns and scarring, partial blindness, and incomplete spinal cord injury that impact his balance and ability to walk. Anderson spent more than 6 months in the hospital. His case manager arranged for an upper limb prosthetist and occupational therapist to collaborate with inpatient therapists to better prepare Anderson for prosthetic rehabilitation.
In July, Anderson was released to return home and begin prosthetic fitting and rehabilitation. Over the course of 1 week, he had myosite training, an expedited prosthetic fitting, and basic prosthesis training, and went home with a functional preparatory prosthesis on his left side. Anderson was able to pick up a cup of water and bring the straw to his lips for a drink for the first time since his accident; he also peeled and ate a banana. His occupational therapist has completed a home assessment to suggest modifications that would enable Anderson to become more independent. His prosthetic rehabilitation will continue with fitting a preparatory prosthesis on his right side, more basic prosthetic training and, eventually, advanced prosthetic training that can lead to significant increases in independence and personal mobility.
“Ultimately, I am hoping for activity-specific prostheses that help me get back out to work in my shop and mess around with cars,” Anderson says.
IN CONCLUSION
Across the stages of upper limb prosthetic rehabilitation, occupational therapists are addressing psychosocial concerns, residual limb changes, and other physical issues that fluctuate throughout the healing process. The challenges therapists face may include the traumatic nature of the loss, the need for a comprehensive team approach, and limited access to medical professionals who are knowledgeable in caring for this relatively small patient population. It is beneficial to enlist input from resources with extensive experience in treating upper limb loss patients in overcoming some of the unique obstacles these patients face.
In most cases, people with upper limb loss or difference are active and productive individuals. The broad range of needs these patients present offer therapists a challenging and exceedingly fulfilling professional experience.
Tiffany Ryan, MOT, OTR, CSCS, has 15 years of professional experience. She is the national director of therapeutic services for Advanced Arm Dynamics. She supervises a nationwide team of therapists, integrating therapy and related services into each patient’s upper limb prosthetic rehabilitation process. For more information, contact .
REFERENCES
- Ziegler-Graham K, Mackenzie EJ, Ephraim PL, Travison PL, Brookmeyer R. Estimating the prevalence of limb loss in the United States: 2005 to 2050. Arch Phys Med Rehabil. 2008;89:422-429.
- Adams P, Hendershot GE, Marano MA. Current estimates from the National Health Interview Survey, 1996. Vital Health Stat 10. 1999 Oct;(200):1-203.
- Dillingham T, Pezzin LE, Mackenzie EJ. Limb amputation and limb deficiency: epidemiology and recent trends in the United States. South Med J. 2002;95:875-883.



![Patient Lifts: Balancing Safety with Recovery[Part Two of a Three-Part Series About Standing Systems, Lifts, and Body Weight Support Units]](https://rehabpub.com/wp-content/uploads/2012/03/2012-03_04-01.jpg)

