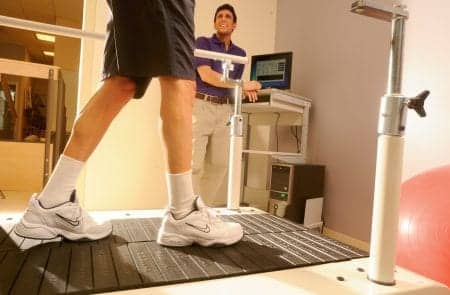
A device with two belts running side-by-side that can be run independently at different speeds is one of the advanced technologies used at the iWalk Recovery Center.
What would you do if you couldn’t walk? To learn about the best practices for gait and balance recovery, it is helpful to imagine one morning you step out of the house, and while walking to your vehicle, you suffer a potentially devastating injury to your brain: a stroke. After lifesaving medical treatments, you learn your rehabilitation program will begin. Though you can use your arm again, and speak and think clearly, you have great difficulty standing and walking. You might find it promising to know that approximately 80% of people who survive a stroke regain the ability to walk, with or without an assistive device.1 Deeper research, however, indicates you may find yourself one of the fewer than 50% of survivors who progress to independent community ambulation.2 Now, you want to know what you can do to harness the power of your brain in helping to recover these functions. After a review of the best practices that follow, imagine how you might create your plan of care for rehabilitation.
ASSESSMENT OF GAIT AND BALANCE
Stroke survivors who arrive at Sheltering Arms, the acute rehabilitation hospital where I work as a physical therapist, often need to relearn how to walk. Sheltering Arms has created a program of inpatient and outpatient services that implements the latest evidence for assessment and intervention called the iWalk Recovery Center. The first step in evaluating a patient’s prospects for functional recovery is to determine what impairments most limit the ability to walk and maintain balance. Are there deficits related to strength and range of motion? Is there involuntary movement, or spasticity, that keeps the affected limb from moving appropriately? Does the individual respond appropriately to balance challenges? Some of these areas make a bigger impact on walking than others, and the answers to these questions often guide the treatment plan.
Identifying the key elements for independent community ambulation can help achieve optimum assessment of gait and balance. A basic function of walking is the ability to perform a reciprocal stepping action. This may be limited among individuals who have suffered a stroke for one of the following reasons: impaired ability to support the body against gravity; inability to move the lower limb; inability to sustain muscle contraction; or impaired spatial awareness. If stroke survivors can step with both legs, then they also must be able to maintain balance during movement of the body forward, as well as adapt to the environment. These functional abilities can be tested with standardized outcome measures for gait and balance, such as the BERG Balance Scale, Dynamic Gait Index, Ten Meter Walk Test, and Timed Up and Go.
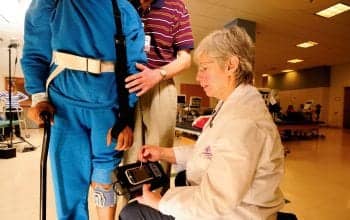
A clinician programs an FES device for a patient at Sheltering Arms. The device can provide feedback to patients trying to figure out “how” to move.
EVIDENCE-BASED TREATMENT
After a thorough assessment to determine factors related to walking and balance, and after developing an understanding of the stroke survivor’s own goals, a treatment plan is initiated. The iWalk Recovery Center utilizes a practice guideline to implement the use of innovative technologies related to the recovery of walking and balance. The use of these technologies is based on principles of motor learning and neuroplasticity. It was not always known that the brain is capable of modifications after injury. I advise patients that most importantly, stroke survivors need to specifically practice the task of walking in an intense, novel, and repetitive way. I also advise that by practicing walking they may experience errors from which the neural pathways will be stimulated to learn.3,4 In addition, they will be exposed to progressive balance challenges to reintegrate balance reactions into functional abilities. As I explain to patients about the physical demands associated with regaining the ability to walk, I introduce them to technology used to aid in this process. Advanced technology allows patients to put these principles into use while a therapist skillfully determines which technology will work for a patient at any given point in recovery—ie, right patient, right tool, right time.
Certain tools are available to help patients perform exercises essential to gait and balance recovery. Behrman and Harkema describe four principles of locomotor training that explain how walking can be task-specific: 1) Weight-bearing must be maximized in the lower extremities, 2) kinematics, or movement of the body and limbs, must be normalized, 3) sensory feedback and input must be maximized, and 4) compensation through use of altered patterns or devices should be minimized.5 Technology can be useful to make walking retraining task-specific, even when a stroke survivor is unable to stand or move the involved limbs. For instance, we may put a patient in a robotic device that stabilizes the body and assists or performs movement of the lower extremities. Sheltering Arms uses robotic-assisted gait training to help a severely impaired individual walk several hundred feet instead of only a few steps. The device provides control of variables such as the amount of body weight support, treadmill speed, and amount of guidance of the lower extremities. All can be modified to progress the intervention within the robot.
An excellent way to improve kinematics and sensory feedback for walking training is to apply functional electric stimulation (FES) to the lower leg to prevent toe dragging. Sheltering Arms frequently uses an FES device designed to work by applying electrodes to the muscle and nerve that flex the foot up at just the right time during walking. Often a patient simply needs to figure out “how” to move his or her body, and the FES device is designed to provide that feedback. After using the device, stroke patients sometimes remark: “Oh, that is what I am supposed to do.” This technology can provide therapists the freedom to get patients practicing task-specific walking earlier. We observe patients are often more engaged and have less fear of falling.
Newer research shows that more intense tasks produce neurophysiologic changes in the brain.6 Repetition is also known to be important in optimizing benefits of neuroplasticity for stroke recovery.3 By applying advanced technology that provides body weight support (BWS), a therapist can completely transform the type of walking practice performed. BWS systems have been used with a treadmill for many years, but new systems allow walking over ground with a ceiling-mounted track for more adaptability in walking practice. The BWS system used by Sheltering Arms staff provides therapists much more freedom to let patients move on their own. That freedom allows therapists to increase the difficulty of the task the patient is performing while maintaining safety for the patient and therapist.
When individuals commit errors while attempting to learn new tasks, it is natural for those errors to actually help improve performance of the new task. Currently, researchers are studying whether the brain will better learn how to produce corrections and permanent adaptations by having a therapist induce or magnify an error. One technology included in this study is the split-belt treadmill. The split-belt device used at the iWalk Recovery Center is engineered with two belts running side-by-side that can be run at the same speed or independently at different speeds. Initial research is promising in demonstrating changes in gait over ground after a stroke survivor practices walking faster while only the lower extremity is taking a shorter step. The result is often a more symmetrical pattern.7
DISCOVER WHAT IS POSSIBLE
The future seems to promise more advanced medical treatment of stroke, and a greater ability to detect and enhance changes in a damaged brain. Through the use of evidence-based assessment and interventions performed by a physical therapist, augmented with advanced technologies, you can discover what is possible when you harness the power of the brain.
Amber Devers, PT, DPT, C/NDT, is a staff physical therapist at Sheltering Arms Physical Rehabilitation Hospital in Mechanicsville, Va. She is an APTA credentialed clinical instructor and member of the Neurology section. For more information, contact
References:
- Gresham GE, Duncan PW, Staston WB, et al. Post-stroke rehabilitation guideline panel. Post-stroke rehabilitation. Clinical practice guideline No. 16 CAHCPR Publication No. 95-0662), Rockville, MD: U.S. Department of Health and Human Services, Public health service, agency for health care policy and research, May 1995.
- Perry J, Garrett M, Gronley JK, Mulroy SJ. Classification of walking handicap in the stroke population. Stroke. 1995;26:982-989.
- Fisher BE, Sullivan KJ. Activity-dependent factors affecting poststroke functional outcomes. Top Stroke Rehabil. 2001;8:31-44.
- Kleim JA, Jones TA. Principles of experience-dependent neural plasticity: implications for rehabilitation after brain damage. Jour Speech, Lang, Hearing Res. 2008;51: 225-239.
- Behrman AL and Harkema SJ. Physical rehabilitation as an agent for recovery after spinal cord injury. Phys Med Rehabil Clin N Am. 2007;18:183-202.
- Kwakkel G. Impact of intensity of practice after stroke: issues for consideration. Disabil Rehabil. 2006: 823-830.
- Reisman DS, Wityk R, Silver K, Bastian AJ. Locomotor adaptation on a split-belt treadmill can improve walking symmetry post-stroke. Brain. 2007; 130: 1861-1872.