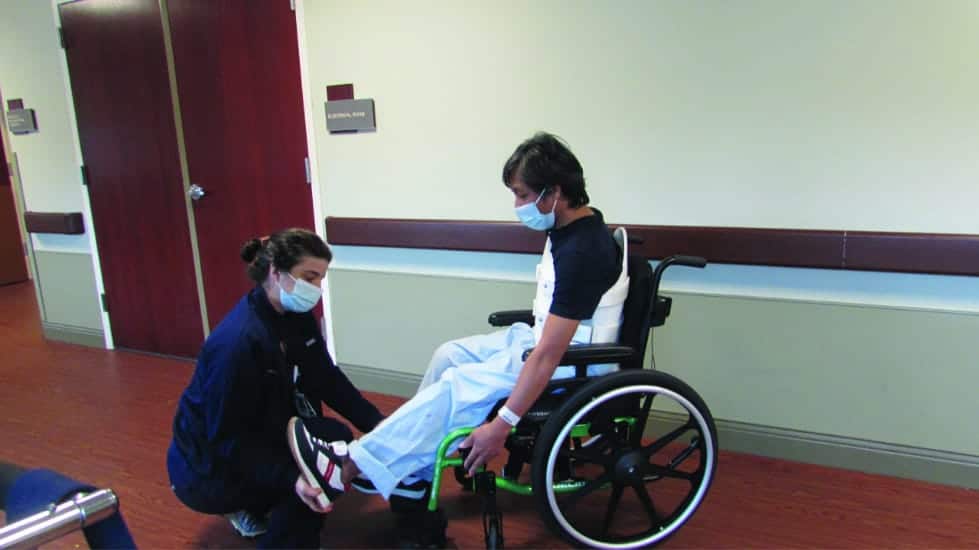
PHOTO CAPTION: Determining the ideal wheelchair prescription for a client with acute SCI requires that a full team of experts work together. Accurate measurements and assessments are crucial as they can impact the choices made, including those for seating and positioning.
An interdisciplinary approach to customized seating and positioning during wheelchair prescription for acute SCI.
By Michelle S. Davidoff, OT, and Sarah Laubengeyer, PT, DPT
Currently there are approximately 294,000 people living in the United States with a spinal cord injury (SCI) and approximately 17,810 new spinal cord injuries each year in the United States. These people may find themselves unable to walk and unable to complete their activities of daily living (ADLs). Physical and occupational therapists work to restore a client’s independence and quality of life through wheelchair prescription. This article will take you through the clinician and client’s collaboration to determine the most appropriate seating and positioning solutions for a client’s new wheelchair. Utilizing an interdisciplinary approach is essential in the acute rehabilitation setting when determining the optimal wheelchair and all of its components for an individual who has sustained an acute complete SCI.
Members of the Team
Members of the treatment team for a patient with SCI will include occupational therapists (OT), physical therapists (PT), a certified assistive technology professional (ATP), and the client. The treatment team will all assist with evaluating and guiding the client through the new seating system selection process. Each member of the team provides an individualized assessment of the client’s mobility, ADL, instrumental activities of daily living (IADL), and client-specific goals. All members must work together for the common goal of promoting independence and improving the client’s overall quality of life. They will all be involved in conducting a home evaluation; posture evaluation; and trials of various wheelchairs, backrests, and cushions.
Level of SCI Injury
Considerations for determining the best seating system include identifying the SCI client’s extent and level of injury. An accurate assessment can be obtained using the International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) as the gold standard for assessment of the patient’s ASIA (American Spinal Cord Injury) level. This scale will tell us the motor and sensory level of injury as well as if a client’s injury level is complete versus incomplete and give us more information regarding the client’s prognosis and potential for recovery. For the purposes of this article, we will focus on an individual who presents as an ASIA A complete injury or an ASIA B incomplete injury with limited motor ability below their injury level.
Social History
The client, family, and members of the treatment team should first meet to discuss the current home setup to ensure wheelchair accessibility in the home and community. Items to consider include steps to enter the home, door and hallway widths, and location of the client’s bedroom and bathroom. A home evaluation form is provided to the caregiver to complete prior to the scheduled wheelchair evaluation. It should include specific measurements to identify wheelchair accessibility. Therapists should also encourage use of pictures to help get a better understanding of the home setup, including the bedroom, bathroom, and front entrance. The types of client homes will vary to include rural vs urban environments with sidewalks.
Accessibility to both the home and community should be discussed prior to ordering a custom wheelchair. Typically, the ASIA A or ASIA B SCI client will require ramp accessibility in the long term to maximize functional independence if entering the client’s home requires walking up steps. Other things to consider include the client’s support system, caregiver availability, and the client’s personal life roles including professional, personal, and family roles. Knowing their life roles will help in determining the most appropriate type of custom wheelchair for your client.
Risk for Skin Breakdown in SCI
Clients living with spinal cord injuries are at increased risk for skin breakdown. Therefore, pressure injury prevention is essential when determining what type of cushion is needed in a wheelchair. The client’s risk can be formally assessed via use of the Braden Scale Score. This outcome measure rates clients at risk for skin breakdown based on factors including sensation, activity, mobility, moisture, shear, and nutrition, and generates a number placing the client into a risk category.
Patients scoring an 18 or below are at risk for skin breakdown and are recommended to utilize a pressure relief cushion. Clients who have an existing pressure injury to the ischial tuberosity, sacrum, or coccyx should be provided specialty cushions for wound healing. Both written and picture documentation of the wound by the client’s medical doctor or certified wound nurse can assist in helping with insurance to cover the cost of a specialty cushion.
Air Cushions
Having a basic understanding of wheelchair cushion types can be helpful in your decision-making process for the SCI patient. Determining the need for stability and pressure relief can further assist your decision-making process. Air cushions, for example, consist of compartments of air that provide immersion of bony prominences such as the ischial tuberosity, sacrum, coccyx, and greater trochanters. These cushions provide the best available pressure relief and should be considered for clients at high risk for skin breakdown (ie, Braden score of 10-12 or with an existing stage 4 or unstageable wound). Possible barriers to this selection would include the need for weekly maintenance by the client or the client’s caregiver, reduced stability during transfers, and increased cost. Insurance companies will not typically cover an air cushion unless the patient has a stage 4 pressure injury.
Gel Cushions
Gel cushions offer the second-best form of pressure relief with added benefits of stability for sitting balance and transfers. Gel cushions offer envelopment of bony prominences via a gel sacral well that is moldable to the client’s body. A possible negative aspect of these cushions is that they have increased weight which can increase energy demands of propulsion. The hybrid versions can significantly reduce the overall weight of the seating system to improve the client’s efficiency with propulsion while adding adequate pressure relief.
Foam Cushions
Foam cushions can be an additional option, but not every foam cushion is made equally. Typically, if your goal for a client is to have low maintenance and low cost, a high-density foam cushion with contour and cutouts will provide the best pressure relief in this category. Considerations should include the client’s mobility level and current and future abilities to complete pressure relief. If ordering a foam cushion, it’s important to ensure that intact skin is present at evaluation.
Living with a SCI, a client will need to complete pressure relief every 15-30 minutes for 1-2 minutes to restore perfusion to the area of skin at the seat interface. It is important to assess your client’s ability to weight shift early in the acute rehabilitation setting. Identifying your client’s ability to complete an active weight versus the need for dependent assistance from a caregiver is crucial in wheelchair and cushion selection. Identifying the presence of a caregiver can also further guide your decision toward power and other assistive technology options to maximize patient independence. Anticipating what your client’s ability and needs will be at 6 months post-discharge can be challenging, and often clinical assessment begins with the patient’s current needs and ability level and prognosis for recovery.
Mobility and ADLs
Physical therapists and occupational therapists work together to determine the mobility needs and strategies for ADL and IADL performance for maximizing the client’s independence. The client’s ability to propel a wheelchair to complete ADL and IADL tasks is a main priority. Clients’ ability and positioning needs during completion of ADLs such as bladder management can further impact the wheelchair selection. For example, a reclining seat may be beneficial for females during self-catheterization techniques. Physical therapists will determine the client’s ability to propel with a standard hand rim or need for additional modifications such as hand rim projections or further power assist options.
Identifying the type of transfer your client utilizes throughout the day will also help to determine an appropriate seating system. Different techniques can include use of a transfer board where removable arm rests would be important versus use of a mechanical Hoyer lift where a tilt-in-space wheelchair could be beneficial.
Mat Evaluation for SCI Patients
Prior to wheelchair evaluation with an ATP, the therapy team will assess and measure all of the client’s anatomical dimensions, strength, range of motion, muscle tone, and postural asymmetries. If postural asymmetries are present, identification of flexible versus fixed posture is determined and utilized for cushion selection. If a client has increased muscle tone, this can lead the team to choose spring-loaded, angle-adjustable footplates and leg rests. Limited hamstring length is common and brings the pelvis into posterior pelvic tilt, which will need to be accommodated in the wheelchair prescription. Assessing the client’s sitting balance in both static and dynamic reaching activities will further assist with the wheelchair prescription and help identify the need for lateral support, dump angle (the inclination of the seat relative to horizontal), or chest straps to ensure safe and comfortable positioning. All of these considerations are important to pressure distribution.
Wheelchair Trial Period
To find the best solution for your client, it’s important to try out different options for not just seating options, but the wheelchair itself.
Ultra-Lightweight Wheelchairs
Often our clients will be ordered an ultra-lightweight wheelchair. The base of an ultra-lightweight wheelchair can weigh no more than 30 pounds and is made of titanium or aluminum. The lightweight feature of the wheelchair allows for easier propulsion, requiring the client to expend less energy and prevent fewer long term upper extremity repetitive strain injuries that may occur from propelling a heavier chair.
Manual Wheelchairs
Manual wheelchairs can come with a rigid frame design or a foldable design. A rigid frame allows for more energy conservation from the client while propelling the wheelchair. A foldable frame wheelchair allows for easier transport of the wheelchair in a car as well as easier storage of the wheelchair when not in use.
A manual tilt-in-space wheelchair allows the client to tilt back up to 55 degrees. This may be a good option for a client who has a current pressure injury and requires a dependent weight shift. This option may also be most appropriate for clients who are experiencing hypotension and require frequent change in position. The cons of a manual tilt-in-space wheelchair include a reduced level of independence, increased reliance on the caregiver, and the significantly increased weight of the wheelchair, making transportation difficult without a specialty van.
Power Assist Systems
A power assist system can be added to the wheelchair. It is often added to an ultra-lightweight wheelchair to decrease the demands on the client’s wrists, arms, and shoulders to reduce the client’s risk of a repetitive strain injury during propulsion. The power assist system can also allow for a client to use a manual wheelchair system for longer before having to switch to a power wheelchair system. This type of system may be most appropriate for your C7 SCI client who has decreased arm range of motion and strength.
Power Wheelchairs
Power wheelchairs are beneficial options for clients with upper extremity motor control challenges. They can be ordered with different types of drive options such as a standard joystick, head array, or sip-n-puff, along with various joysticks for clients with limited upper extremity range of motion or fine motor coordination. Power wheelchairs can allow for clients to independently control the tilt and recline mechanism for pressure relief. A seat elevator can also be added to the power wheelchair to allow for clients to access overhead cabinets and countertops in their home and work/school environments to promote increased independence with ADL and IADL tasks. A power wheelchair may be a good option for a client with a higher-level cervical SCI. But it is important to note that, similar to the manual tilt-in-space wheelchair, the power wheelchair cannot be transported in a standard car.
Choosing Backrests
You’ll also want to do trials of backrests. These can include custom moldable backrests, rehab backrests, or sling back backrests. It is also important to consider the need for lateral supports when determining what type of backrest is most appropriate for your client. Typically, identifying the presence of a fixed postural asymmetry can lead a therapist to determine a need for a custom moldable backrest. Clients with impaired trunk control may require lateral support to maintain an upright erect trunk to complete propulsion and ADLs. It is important to obtain accurate anatomical measurements to ensure that the backrest does not impede the movement of the client’s shoulder blades during wheelchair propulsion, especially for the client who will use propulsion as a primary means of mobility.
Wheelchair Evaluation
On the day of the wheelchair evaluation with the ATP, members of the team including the occupational therapist, the physical therapist, the client, and the caregiver should be present. A home evaluation form; posture evaluation; and trials of various wheelchairs, backrests, and cushions should have already been completed. This level of preparation will allow for an efficient wheelchair evaluation and facilitate the best outcome for the client. The ATP will assist the client in ordering all portions of the permanent seating system.
Michelle S. Davidoff, OT, has been an occupational therapist working in an acute rehabilitation setting for the last 19 years. She has specialized in the treatment of patients with spinal cord injuries throughout her career and has taken a special interest in assisting these patients with custom wheelchair prescription. She currently works in the wheelchair clinic at the Kessler Institute for Rehabilitation in Marlton, NJ. She obtained her BS in Occupational Therapy from the University of Pittsburgh as well as an MS in Occupational Therapy from Temple University.
Sarah Laubengeyer, PT, DPT, has worked in acute rehabilitation for 6 years and has a special interest in wheelchair prescription and cushion selection. She currently works in the wheelchair clinic at the Kessler Institute for Rehabilitation in Marlton, NJ, and is on a hospital-wide committee for pressure injury prevention.
References
- Hornby TG, Reisman DS, Ward IG, et al. Clinical practice guideline to improve locomotor function following chronic stroke, incomplete spinal cord injury, and brain injury. J Neurol Phys Ther. 2020;44(1):49-100. doi: 10.1097/NPT.0000000000000303
- Chafetz RS, Gaughan JP, Vogel LC, Betz R, Mulcahey MJ. The international standards for neurological classification of spinal cord injury: intra-rater agreement of total motor and sensory scores in the pediatric population. J Spinal Cord Med. 2009;32(2):157-161. doi: 10.1080/10790268.2009.11760767
- Sadeghi Fazel F, Derakhshanrad N, Yekaninejad MS, Vosoughi F, Derakhshanrad A, Saberi H. Predictive value of braden risk factors in pressure ulcers of outpatients with spinal cord injury. Acta Med Iran. 2018;56(1):56-61.
- Brienza D, Kelsey S, Karg P, et al. A randomized clinical trial on preventing pressure ulcers with wheelchair seat cushions. J Am Geriatr Soc. 2010;58(12):2308-2314. doi: 10.1111/j.1532-5415.2010.03168.x
- Jean L Minkel. Seating and mobility considerations for people with spinal cord injury. Physical Therapy. 2000;80(7):701–709. doi: 10.1093/ptj/80.7.701
- Regan MA, Teasell RW, Wolfe DL, et al. A systematic review of therapeutic interventions for pressure ulcers after spinal cord injury. Arch Phys Med Rehabil. 2009;90(2):213-231. doi: 10.1016/j.apmr.2008.08.212
- Vos-Draper TL, Morrow MMB. Seating-related pressure injury prevention in spinal cord injury: a review of compensatory technologies to improve in-seat movement behavior. Curr Phys Med Rehabil Rep. 2016;4(4):320-328. doi: 10.1007/s40141-016-0140-7
- Jan YK, Jones MA, Rabadi MH, Foreman RD, Thiessen A. Effect of wheelchair tilt-in-space and recline angles on skin perfusion over the ischial tuberosity in people with spinal cord injury. Arch Phys Med Rehabil. 2010;91(11):1758-1764. doi: 10.1016/j.apmr.2010.07.227
- State Spinal Cord Injury Service. Prescribing manual wheelchair with propulsion assist devices. Agency for clinical innovation 2022. Available at: https://aci.health.nsw.gov.au/networks/spinal-cord-injury/spinal-seating/module-9/prescribing-manual-wheelchair-with-propulsion-assist-devices. Accessed 2/17/2022.
- Yang YS, Koontz AM, Yeh SJ, Chang JJ. Effect of backrest height on wheelchair propulsion biomechanics for level and uphill conditions. Arch Phys Med Rehabil. 2012;93(4):654-659. doi: 10.1016/j.apmr.2011.10.023
- Michael E, Sytsma T, Cowan RE. A primary care provider’s guide to wheelchair prescription for persons with spinal cord injury. Top Spinal Cord Inj Rehabil. 2020;26(2):100-107. doi: 10.46292/sci2602-100
Related Content:
Evaluate, Adapt, and Succeed in Seating and Positioning
Getting the Right Fit: Seating and Positioning