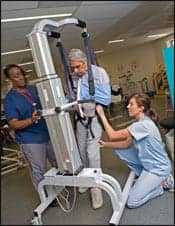
Michelle Terrell, PT, completes static balance training with a vestibular rehabilitation patient. Desired outcomes include increased stance duration and decreased postural sway.
by Sandra Nagel, MPT, and Michelle Terrell, MS, PT
Dizziness and imbalance affect a large percentage of people and can significantly limit functional mobility. According to some studies, dizziness affects 13% to 38% of older adults in the United States depending on the population specified. A 2005 study states that 61% of the inner city geriatric population reports dizziness. Clearly, dizziness and imbalance are common problems for people, whether or not treatment is sought. Vestibular rehabilitation is often an effective treatment for restoring function and decreasing symptoms.
At Mary Free Bed Rehabilitation Hospital in Grand Rapids, Mich, the facility’s focus is on restoring hope and freedom, which extends to a specialty program for people who are affected by vestibular and balance dysfunction. The hospital’s vestibular rehabilitation program has been in place for more than 20 years. Approximately 150 patients are seen annually for vestibular rehabilitation through Mary Free Bed’s outpatient program. Also, the facility’s therapists who specialize in vestibular rehabilitation treat more than 175 additional people with vestibular dysfunction each year through Mary Free Bed’s post-concussion program.
The vestibular system senses rotational and linear movement of the head. This information is processed by the brain to allow the body to remain in a desired position with steady visual interaction with the environment. Vestibular disorders arise from dysfunction within the inner ear and/or brain caused by injury, infection, or disease that alters the function of this sensory processing system. Vestibular disorders can lead to decreased balance, reduced activities of daily living, increased potential for falls, and increased risk for depression. Physical therapy—specifically, vestibular rehabilitation—has been shown to be effective in treating vestibular dysfunction.
Defining the Dysfunction
There are several types of vestibular dysfunction. Part of the role of a vestibular rehabilitation specialist, such as a physical therapist, is to help the medical team determine the source of a patient’s dizziness or vertigo. Vestibular disorders can include but are not limited to benign paroxysmal positional vertigo (BPPV), Labyrinthitis/vestibular neuritis, Meniere’s disease, acoustic neuroma, and post-concussive vestibulopathy. In general, vestibular problems occur due to trauma, viral infection, or central nervous system disorder.
BPPV is a mechanical disorder of the inner ear that presents as brief, acute periods of true vertigo or spinning dependent on changes of head position. Traditionally, the Epley maneuver is the gold standard technique used to treat BPPV. Labyrinthitis/vestibular neuritis is an acute vestibulopathy that can follow illness such as an upper respiratory infection or gastroenteritis. Vestibular neuritis often presents with severe rotational vertigo associated with head movement during the acute phase and as hypofunction of the vestibular system in the chronic state. There can be associated hearing loss or tinnitus.
Meniere’s disease is characterized by devastating hearing loss and vestibular symptoms that are recurrent in nature and may include pressure or fullness in the ear, altered low-frequency hearing, tinnitus, rotational vertigo, postural imbalance, nystagmus, and nausea. Therapy treatment is typically completed between exacerbations to restore any residual impairments.
A concussion is a type of mild traumatic brain injury resulting from injury to the head or body that causes sudden movement of the head back and forth. The injury may cause changes in brain chemistry and function at a cellular level. Concussions frequently result in cognitive problems, headaches, neck pain, or double or blurry vision. Balance problems, dizziness, and the traumatic onset of BPPV are also common following concussion.

There are multiple technologies to enhance diagnosis and treatment of vestibular dysfunction. Here, Sandra Nagel, PT, educates a patient for completion of a dynamic balance assessment on a testing device.
Testing and Treatment
Physical therapy can assist in treating many vestibular disorders and hasten the return to prior level of function. At Mary Free Bed Rehabilitation Hospital, the referral process traditionally includes a prescription from a physician as a starting point. Direct access has allowed some patients to connect with a vestibular specialist without physician referral. During evaluation, three main components of vestibular function are assessed, including visual-vestibular interaction, static and dynamic balance ability, and sensitivity to positional change.
Visual-vestibular interaction assessment allows the therapist to identify symptoms—primarily, dizziness with smooth pursuit tracking, saccades, and vestibulo-ocular reflex (VOR) tasks. Training with those tasks in a progressive manner occurs in vestibular rehabilitation until a patient is symptom-free, which allows for improved function such as driving or being in busy visual environments.
Static and dynamic testing addresses patients’ ability to maintain balance during a variety of situations. For example, static balance may include normal and narrowed base of support stance tests. For dynamic balance assessment, ambulation with head movements and pivot turns are part of the test battery.
Positional change testing investigates sensitivity to rapid head or body movements such as head turns, nods, standing pivots, rolling, and sitting up or lying down quickly. Treatment in this area could include repositioning techniques or habituation training to assist in decreasing sensitivity to positional change.
At Mary Free Bed Rehabilitation Hospital, completion of computerized dynamic posturography is regularly a part of vestibular rehabilitation to provide more quantitative, objective information regarding a person’s balance abilities. Computerized dynamic posturography uses force plate technology to measure the center of pressure during a variety of conditions that challenge a person’s balance. The primary goal of completing computerized dynamic posturography is to create measurable data that can identify change. Tests evaluate a person’s response to differing sensory conditions and changes in the support surface. Both voluntary and involuntary movement responses can be analyzed. The test results can help the clinician identify which sensory condition may be the source of the patient’s dizziness or imbalance symptoms.
Once a pattern of dysfunction is identified with computerized dynamic posturography, a treatment plan specific to the patient’s needs can be developed. Customized training can occur on the same apparatus where testing was completed. Alternatively, training can be completed using a variety of other devices common in physical therapy, such as balance boards and foam cushions. A home exercise program can also be developed in which a person trains a variety of conditions such as eyes open versus eyes closed, as well as stances on differing surfaces or with differing bases of support.
Videonystagmography (VNG) technologies are used for testing inner ear and central vestibular processing abilities. VNG measures the movements of a person’s eyes using infrared cameras affixed to goggles that are worn during testing. VNG can also help determine whether the inner ear dysfunction is unilateral or bilateral. Typically, VNG tests monitor for nystagmus or rapid eye movements during steady gaze or specific gaze-related tasks, nystagmus during specific positions or changes of position, and nystagmus during caloric testing. The visual tests evaluate a patient’s ability to complete specific gaze-related tasks and allow a practitioner to evaluate the patient’s central processing abilities. The positional change testing portion of VNG can help identify symptoms of BPPV or nystagmus when a patient is moved into specific positions.
Finally, caloric testing is completed to identify whether both right and left vestibular organs are appropriately responding to input. During this test, either warm or cold air is circulated through a small, soft tube inserted into the ear canal. The practitioner can identify if the vestibular system is correctly functioning by observing the patient’s eyes.
Rotational chair assessment can be incorporated into evaluation of vestibular function. It is often utilized in conjunction with VNG testing to help confirm a specific diagnosis and increase overall accuracy of testing. The purpose of rotary chair testing is to determine whether the vestibular system or the central processing system is the source of the problem the patient is experiencing. This testing is considered the “gold standard” for identifying bilateral vestibular hypofunction and central nervous system compensation. During rotary chair testing, the patient sits in a chair that spins to mimic normal head velocities during daily life. Additionally, the patient may view moving stripes while seated in the chair so the practitioner can assess any dizziness that may be created by visual input. Finally, the patient views a dot that moves with the patient while the chair is being rotated.
Goal Setting and Recovery
Not all who need vestibular rehabilitation require the described technological tests. Often, those tests are done under supervision of physicians who are ear, nose, and throat specialists or neurotologists. Many patients are referred from primary care physicians or neurologists for vestibular rehabilitation. In cases where specialized testing is not indicated, clinical balance and vestibular assessments are completed. Patients can always be referred for more specialized testing.
From the various sources of testing, the treatment plan is set and the home exercise program is developed specific to each patient. Goals for treatment incorporate a patient’s problem areas with expectations for improvement. For example, increased balance stance durations with decreased amounts of sway and habituation of dizziness with rapid position changes may be goals. Improved dynamic balance, such as walking with head movement, is another common goal. The ultimate goal is maximizing function by decreasing or eliminating dizziness symptoms by discharge.
Vestibular rehabilitation is an effective and evidence-based means of improving function while decreasing symptoms of dizziness and imbalance. Most often, dizziness symptoms are not visible to others, and yet people who experience vestibular problems suffer, sometimes for a long periods of time before receiving help. For many, being treated by a vestibular rehabilitation specialist is key for recovery from balance and dizziness disorders. RM
Sandra Nagel, MPT, is a physical therapist at Mary Free Bed Rehabilitation Hospital in Grand Rapids, Mich. She has practiced for 20 years, always in neurological rehabilitation. Her current caseload is made up of post-concussive and vestibular patients. She graduated from Oakland University.
Michelle Terrell, MS, PT, is a physical therapist at Mary Free Bed Rehabilitation Hospital in Grand Rapids, Mich. She has been in practice for 14 years and worked with a variety of patients with musculoskeletal and neuromuscular disorders. She currently focuses on vestibular rehabilitation and treatment of post-concussive disorders. She is a graduate of Grand Valley State University. For more information, contact [email protected].
Bibliography
- Alrwaily M, Whitney SL. Vestibular rehabilitation of older adults with dizziness. Otolaryngologic Clinics of North America. 2011;44(2):473–496. doi:10.1016/j.otc.2011.01.015.
- Helminski JO, Janssen I, Kotaspouikis D, et al. Strategies to prevent recurrence of benign paroxysmal positional vertigo. Arch Otolaryngol Head Neck Surg. 2005;131(4):344. doi:10.1001/archotol.131.4.344.
- Helminski JO, Zee DS, Janssen I, Hain TC. Effectiveness of particle repositioning maneuvers in the treatment of benign paroxysmal positional vertigo: A systematic review. Phys Ther. 2010;90(5):663–678. doi:10.2522/ptj.20090071.
- Alrwaily M, Whitney SL. Vestibular rehabilitation of older adults with dizziness. Otolaryngologic Clinics of North America. 2011;44(2):473–496. doi:10.1016/j.otc.2011.01.015.
- Herdman S, Clendaniel R. Vestibular Rehabilitation. United States: F.A. Davis Company; September 1, 2014.
- Hall SF, Ruby RRF, McClure JA. The mechanics of benign paroxysmal vertigo. J Otolaryngol. 1979;8(2):151–158.
- Oghalai JS, Manolidis S, Barth JL, Stewart MG, Jenkins HA. Unrecognized benign paroxysmal positional vertigo in elderly patients. Otolaryngol Head Neck Surg. 2000;122(5):630–634. doi:10.1016/s0194-5998(00)70187-2.
- Hillier SL, McDonnell M. Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Cochrane Database Syst Rev. 2011;(2).
- Hain TC. Neurophysiology of vestibular rehabilitation. NeuroRehabilitation. 2011;29:127–141.
- Videonystagmography | national dizzy and balance center | NDBC. http://www.nationaldizzyandbalancecenter.com/services/balance-lab-testing/videonystagmography/. Accessed January 4, 2016.
- Hain TC. Rotatory chair testing. http://www.dizziness-and-balance.com/testing/ENG/rchair.html. Accessed January 4, 2016.
- Rotational chair | national dizzy and balance center | NDBC. http://www.nationaldizzyandbalancecenter.com/services/balance-lab-testing/rotational-chair-testing/. Accessed January 4, 2016.
- Latest news. http://vestibular.org/. Accessed January 4, 2016.
- Natus Medical Incorporated. http://www.natus.com/. Accessed January 4, 2016.