 |
| Richard E. Joreitz, PT, DPT, ATC |
Physical agents, alone or in tandem, can prove useful tools for treating sports/weekend warrior injuries when paired with therapeutic goals such as alleviating inflammation, swelling, stiffness, and multiple physiological problems.
“This is a hot topic in the physical therapy world—a lot of people use modalities as a main gateway for treatment, for getting better, whereas they should really be used as an adjunct only,” says Richard E. Joreitz, PT, DPT, ATC, physical therapist, and adjunct instructor in the Department of Physical Therapy, UPMC Center for Sports Medicine, Pittsburgh. “Modalities are not going to fix any underlying problems. There should be appropriate strengthening and stretching exercises and appropriate use of manual therapy to treat musculoskeletal injuries.”
LASERS
Lasers can help promote healing both superficial and deep, and the modality is very effective with acute and chronic pain with or without inflammation, says physical therapist Tom Watson, DPT, MEd, DAAPM, Peak Performance Physical Therapy, Redmond, Ore. The type used in physical therapy is low-level, helium-neon lasers, which are 632.8 nanometers. In his practice, Watson favors infrared lasers, or gallium arsenide lasers, which are 830 nanometers. As the laser penetrates, it stimulates the mitochondria in each cell, which then releases ATP. “The ATP is released at an increase of 150% to 1,000%, depending on the tissue, resulting in increased activity of Krebs cycle,” says Watson, past president and cofounder of Pain Management SIG, American Physical Therapy Association. More information is found at www.laser.nu.
Some studies have found that low-level laser has a positive effect on pain, says Elizabeth Oakley, MSPT, DHSc, associate professor of physical therapy, Andrews University Department of Physical Therapy, Berrien Springs, Mich. “I’ve found good results using laser on the acute, inflammatory phase,” she says. “So, when someone is injured, in the first 24 to 72 hours, I’ve seen some improvement with pain and motion when using laser.”
ULTRASOUND

More than 50 million Americans live with chronic pain. Look for information on the latest modalities and technologies to address this demographic on this website.
For someone who has a trigger point, there has been some evidence suggesting that ultrasound in combination with stretching can be helpful, says Oakley. Ultrasound in combination with electrical stimulation has also been helpful in managing pain for different conditions such as arthritis and other inflammatory conditions, she adds.
Ultrasound is used for deep heating effects; it has been shown to increase blood flow, and to increase tendon extensibility prior to performing range of motion exercises, for example, with some Achilles tendons and patellar tendons, says Joreitz. “I’ll tell them right off the bat that the electrical stimulation doesn’t heal anything, but it feels great,” he says. The relief could last 5 minutes to a couple of hours after the treatment ends. Joreitz says there is good evidence for use of high-intensity electrical stimulation for strengthening muscles, ie, quadriceps after knee injury/surgery.
Studies on the effects of ultrasound used for acute and chronic injuries show it is no more effective than heat, and it is short-acting, Watson says, citing two journal articles published in Physical Therapy in 2001, and also in Pain 1995. A February 2009 study shows laser offers a distinct advantage over ultrasound, providing a greater reduction in pain and stimulating the healing of tissue, Watson adds.
ELECTRIC STIMULATION
 |
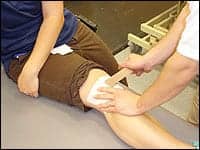 |
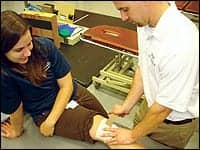
| Richard E. Joreitz, PT, DPT, ATC, Department of Physical Therapy, UPMC Center for Sports Medicine, Pittsburgh, taping a client’s knee. |
Transcutaneous electrical nerve stimulation (TENS) is used for pain relief, and neuromuscular electrical stimulation (NMES) is used for muscle strengthening.
Electricity treatments date to ancient times, when eel currents were applied to treat pain. Electro-stim TENS units are based on milliamps. They use superficial counterirritant types of electricity that work on a gate theory—ie, they block pain at the spinal cord level. Recent studies have shown the modality can provide temporary relief of pain, Watson says. “They work like eyeglasses, so, when you turn it off, your pain will come back,” he says, adding, “there is short-term relief of pain, but it causes no healing of the tissue.” He notes it does not work very well with fibromyalgia. Microcurrent stimulation, which is based on microamperage, causes a profound biophysiological response, working on a cellular level, Watson says. More than 100 studies of microstim show it can be effective for chronic pain, fibromyalgia, and some sports injuries, he says. He uses it transcranially for headaches and acute pain. “It can help with the swelling, and it reduces the intensity of the pain. It works on the dorsal horn of the spinal cord, which alters pain perception and the cognition of pain—resulting in less pain overall,” he says.
THERAPEUTIC TAPING
Athletic-type taping can help stabilize a joint or a specific muscle. Therapeutic taping, which basically involves a variety of single strands of tape, may help improve the proprioception of a given joint, which then results in better movement around the physiological axis.
Patellofemoral pain is common in runners, as well as the everyday person who has pain walking up and down stairs. Joreitz often tapes the patella if it is not tracking properly. If patients benefit from taping, the therapist may explore getting them a brace to stabilize the patella. “So it’s kind of a pathway to see if a brace is going to work rather than spend the money for it,” he says. He also does ankle taping and plantar fasciitis taping. “Anytime I get a patient with an ankle sprain, when they get back into functional training, the first couple of times I’ll tape their ankles to provide some support. They feel confident with it. If somebody has plantar fasciitis, I’ll tape their heels, tape their arches. See if they have relief with that. Commonly they do.”
Oakley uses taping for ankle and knee pain patients. “Maybe the patella isn’t tracking like it should—sometimes taping can help,” she says. It can also help teach patients to maintain a desired posture. “If we tape them in the correct position, when they move out of that position, the tape starts to pull. That reminds them, ‘I need to stay this way.'”
HOT AND COLD THERAPIES
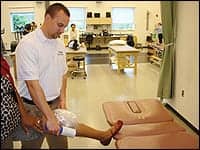 |
| Richard E. Joreitz, PT, DPT, ATC, wrapping a bag of ice on a client’s knee. |
Hot and cold therapies can be very effective for sports enthusiasts and weekend warriors. Cold is most effective during the first 72 hours after an injury, then either mode can be used, or they can be alternated, says Watson. The end result of the heat and cold is the same after about 5 to 7 minutes, when it’s not an acute injury, he says.
Ice provides great analgesia, especially in combination with electrical stimulation, says Oakley. “The two combined have been effective in decreasing pain, and if initiated soon after the injury, electrical stimulation helps to decrease the swelling associated with the acute inflammatory stage as well,” she adds.
IONTOPHORESIS
Physical therapists use a variety of solutions with iontophoresis, which, by use of a patch, drives medications through the skin to deliver an anti-inflammatory medication locally to the injured site, via electricity. Watson says dexamethasone is good for acute inflammatory conditions; magnesium can be used for muscle relaxation; acetic acid for heel spurs; sodium chloride for adhesion; salicylates for edema and pain reduction; lidocaine and bupivacaine for acute sprains, bursitis, and neuritis; and zinc for wound healing.
Iontophoresis does not have to go through the gastrointestinal system. “Rarely will you ever hear a patient complain of it,” says Joreitz. “It used to be there would be a machine and they’d have to sit for 10 to 15 minutes with it, depending on the dosage, but now there are patches you can use and they have to sit there for only 3 minutes.”
TOPICAL GELS AND CREAMS
 |
 |
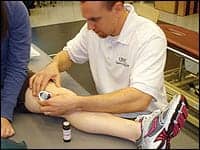 |
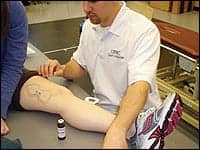
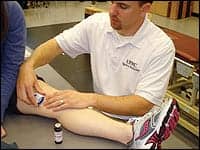
| Physical therapist Richard E. Joreitz, setting up iontophoresis on a client. |
Approximately one-third of adults over 50 sustain injuries and muscle disorders following injuries, which are sometimes severe. The American Pain Foundation in 2008 found that topical gels and creams containing counterirritants were as effective as over-the-counter tablets; they worked as well as the oral versions, and are often less expensive, says Watson, a credentialed diplomate of the American Academy of Pain Management.
CONTINUOUS PASSIVE MOTION (CPM)
CPM, as a component of a patient’s treatment plan, can be beneficial for several treatment goals, such as facilitating return of range of motion, improving lubrication of joints, and reducing the risk for deep vein thrombosis.
Surgeons may instruct their patients to use CPM devices at home following surgery. Joreitz supports their use. “Assuming they’re compliant with it, that means I know they’re increasing their motion,” he says. The device is often used for at least 4 hours a day. It may be helpful for improving ROM, but studies have shown that it is no more effective at improving ROM than exercise, he adds.
BIOFEEDBACK
Biofeedback is the use of an auditory or visual signal to provide the client with feedback of a physiological function. Oakley sometimes uses biofeedback to provide clients with information about the electrical activity of their muscle(s). She has used it with clients who have issues with either relaxing an overactive muscle or triggering a muscle that they may not be activating. “You may have a baseball pitcher or maybe a tennis player and they start developing shoulder issues. Sometimes the scapula does not stabilize appropriately because the surrounding muscles are weak or they are not activated in an appropriate sequence,” she says. “We can use biofeedback in combination with electrical stimulation to train them to contract that muscle at the appropriate time required for the desired physical activity. Once the muscle is strong and the client is able to activate it in a timely fashion, it will help to provide the stability they need to perform their activity.”
It can also help clients who carry a lot of tension in a muscle, which can cause pain. In either case, the visual or auditory signal can alert the client that the muscle is active or, in the case of an overactive muscle, encourage the patient to silence the signal or decrease the visual output.
PROACTIVE APPROACH
Exercise is very important in preventing future injuries. “We use exercise, core strengthening, even strengthening muscles around the joint that is injured to help prevent future injuries and improve performance,” says Oakley. Regimens are tailored to a patient’s needs, their sport, and their activity level, and are specific to the injury itself.
Physical therapists at Peak Performance Physical Therapy perform an evaluation of the patient’s strengths and weaknesses and coordinate activities, applying dosed and specific exercises to stabilize movement around a normal physiological axis, which helps to reduce the chance of injury or trauma to a joint or muscle. To view an informational webinar on pain management, contact .
Judy O’Rourke is the associate editor of Rehab Management. She can be contacted at .





